Keratoconus
🧠 Quick Answer
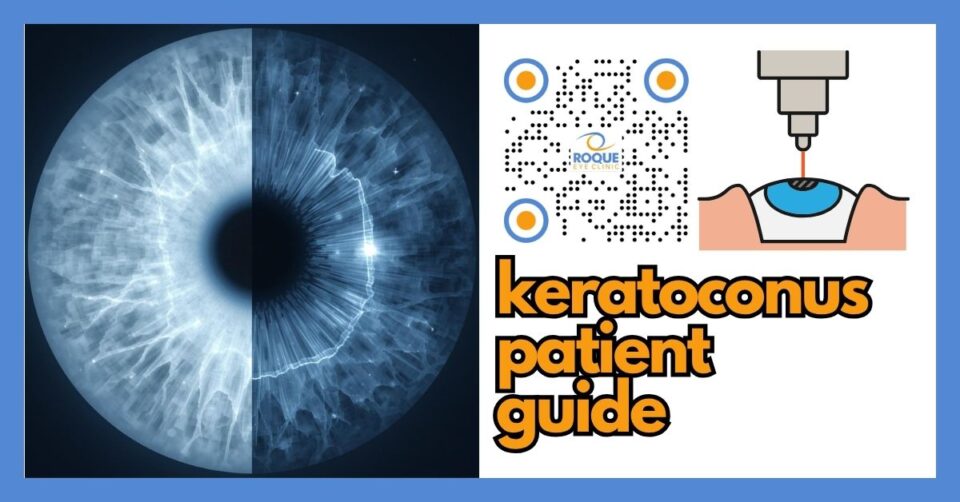
Keratoconus is a condition in which the cornea gradually becomes thinner and bulges forward into a cone-like shape. This can cause blurry vision, ghosting, glare, worsening astigmatism, and frequent prescription changes. Mild cases may be managed with glasses or contact lenses, while progressive cases may need corneal cross-linking, and advanced scarred cases may need corneal transplant surgery.
Keratoconus is one of the most important corneal conditions in refractive surgery because it directly affects the shape and strength of the cornea. A normal cornea is round and smooth enough to focus light clearly onto the retina. In keratoconus, the cornea becomes thinner and more irregular over time. As a result, vision may become distorted, less crisp, and harder to correct with ordinary glasses.
This matters not only for general eye care, but also for refractive surgery screening. A patient with keratoconus or even early suspicious keratoconus may not be a safe candidate for LASIK or other tissue-removing corneal laser procedures. That is why modern corneal topography and tomography are so important before refractive surgery.
🧩 Focus: Keratoconus as a progressive corneal ectatic disorder
👁 Goal: Explain symptoms, diagnosis, progression, treatment options, and why keratoconus matters in refractive surgery screening
🛡 Evidence-Based: Preferred Practice Patterns • Standards of Care • Systematic Reviews • Meta-Analyses
REFRACTIVE SURGERY Knowledge Hub
Start with the complete guide:
🔬 Keratoconus Anatomy Micro-Primer
- Cornea: The clear front window of the eye. It provides much of the eye’s focusing power.
- Corneal stroma: The thick middle structural layer of the cornea. In keratoconus, this layer becomes biomechanically weaker and thinner.
- Corneal apex: The steepest or most protruding part of the cornea. In keratoconus, this area often becomes more cone-shaped and irregular.
- Tear film: The smooth tear layer on the cornea. An unstable surface can worsen blur and make measurements less reliable.
📘 Keratoconus Terminology Glossary
- Keratoconus: A condition in which the cornea thins and bulges outward into a cone shape.
- Astigmatism: Blurred or distorted vision caused by an irregular corneal shape.
- Topography: A map of the cornea’s front surface shape.
- Tomography: A more detailed scan that analyzes both the front and back surfaces of the cornea and its thickness profile.
- Cross-linking: A procedure that strengthens the cornea to help slow or stop progression.
- Corneal scar: Permanent clouding in the cornea that can reduce vision in advanced disease.
Quick Navigation
Related Reading
Key Learning Points
- Keratoconus is a progressive thinning and bulging disorder of the cornea.
- It often begins in the teenage years or young adulthood, though detection can happen later.
- Symptoms may include blurred vision, ghosting, worsening astigmatism, glare, and frequent prescription changes.
- Glasses may help in early disease, but many patients eventually need specialty contact lenses.
- Corneal cross-linking is used to stabilize progressive keratoconus.
- Keratoconus is a major reason why some patients are not good candidates for LASIK.
What Keratoconus Is
Keratoconus is a corneal ectatic disorder. “Ectatic” means the cornea becomes weaker and starts to bulge. Instead of remaining smoothly rounded, the cornea gradually becomes more cone-shaped and irregular. This changes how light enters the eye and often causes increasing myopia, irregular astigmatism, glare, ghosting, and reduced quality of vision.
One simple way to picture it is to imagine a camera lens that is supposed to be smooth and evenly curved. If one area becomes thinner and starts to bulge forward, the image becomes distorted. That is essentially what happens in keratoconus. The issue is not just “needing stronger glasses.” The optical surface itself becomes less regular.
💡 Analogy
A normal cornea is like a smooth clear dome. A keratoconic cornea is more like a dome that has developed a weak spot and pushed outward. Even if the glass stays clear, the image passing through it becomes more warped.
Symptoms
Symptoms can vary from person to person. Early keratoconus may feel like a prescription that never stays stable. Patients may notice:
- Blurred vision
- Ghosting or double outlines around objects
- Increasing myopia or astigmatism
- Frequent need to change glasses
- Glare, halos, or sensitivity to light
- Reduced quality of night vision
- Eye discomfort in advanced cases
Some patients also have itchy eyes, and rubbing may become a harmful habit. In advanced disease, corneal scarring can further reduce vision.
Why It Happens
The exact cause of keratoconus is not fully understood. It is generally thought to involve a combination of genetic predisposition and environmental or behavioral factors. Research and patient information sources frequently mention family tendency, allergies, and eye rubbing as important associations. Not every patient has a family history, and not every eye-rubber develops keratoconus, but repeated rubbing is widely treated as a major risk factor for progression.
For patients, the practical message is simple: if you have keratoconus or are at risk for it, avoid rubbing your eyes and treat allergy or ocular surface irritation properly.
Who Commonly Gets Keratoconus?
Keratoconus is often diagnosed in teens and young adults. That does not mean older adults cannot have it. Some are diagnosed later because their condition was mild earlier, or because modern imaging finally detected subtle disease. Keratoconus may progress for years, then slow or stabilize. The pace is not identical in every patient.
Diagnosis and Tests
Diagnosis starts with a careful eye examination, but modern imaging is extremely important. A patient may be suspected of having keratoconus if they show increasing irregular astigmatism, unexplained best-corrected blur, or frequent prescription changes. Testing often includes:
- Visual acuity testing
- Refraction
- Slit-lamp examination
- Corneal topography
- Corneal tomography
- Pachymetry (corneal thickness measurement)
- Assessment for corneal scarring and ocular surface disease
Topography maps the front of the cornea. Tomography goes further by evaluating both front and back surfaces and thickness patterns. This matters because very early keratoconus may be missed if one relies only on refraction or slit-lamp findings.
Stages and Severity
Keratoconus exists on a spectrum. Some patients have mild disease and function well with glasses or soft toric lenses. Others develop irregular astigmatism that needs rigid gas-permeable, hybrid, or scleral lenses. In more advanced disease, thinning, steepening, and corneal scarring can reduce vision significantly.
The important point for patients is that “keratoconus” is not one fixed level of disease. Your treatment depends on how advanced it is, whether it is progressing, how well you see with glasses or contact lenses, and whether the cornea remains clear.
Treatment Options
1) Glasses
In early keratoconus, glasses may still provide useful vision. However, as the cornea becomes more irregular, glasses often stop giving crisp correction.
2) Contact lenses
Many patients with keratoconus need specialty contact lenses. These may include rigid gas-permeable lenses, hybrid lenses, piggyback systems, or scleral lenses. These lenses do not cure keratoconus, but they can greatly improve vision by creating a smoother optical surface.
3) Corneal cross-linking
Corneal collagen cross-linking is used to strengthen the cornea and reduce the risk of continued progression. This is a major treatment advance because it aims to stabilize the disease, not just sharpen vision temporarily. It is especially important in progressive keratoconus, including in younger patients who may worsen more quickly.
4) Corneal procedures for vision rehabilitation
Selected patients may undergo additional procedures intended to improve corneal shape or vision quality, depending on the case and surgeon’s judgment. These are individualized decisions and are not suitable for every patient.
5) Corneal transplant
In advanced cases with severe scarring, thinning, or poor vision that cannot be adequately managed with lenses, corneal transplantation may be considered. While this sounds intimidating, it is generally reserved for a minority of more advanced cases.
🚨 Emergency Warning
Seek urgent ophthalmic review if you develop sudden severe pain, rapid worsening of vision, marked redness, or a sudden cloudy white appearance of the cornea. Rare acute events such as corneal hydrops can occur in advanced keratoconus and should not be ignored.
Why Keratoconus Matters in Refractive Surgery
Keratoconus is one of the most important reasons a patient may not be a safe candidate for LASIK and similar corneal tissue-removing refractive procedures. If the cornea is already biomechanically weak, removing additional tissue can increase the risk of worsening instability or postoperative ectasia. That is why careful screening with topography, tomography, and pachymetry is essential before refractive surgery.
This does not mean every patient with keratoconus can never have any surgical intervention. It means the treatment plan must be individualized. In many cases, the priority is stabilization with cross-linking and vision rehabilitation rather than elective laser reshaping.
Can Keratoconus Be Prevented?
There is no guaranteed way to prevent keratoconus entirely, especially when genetics are involved. However, there are practical steps that may reduce avoidable worsening:
- Avoid rubbing your eyes
- Treat allergies and itch properly
- Follow up regularly if you have a suspicious corneal scan or family history
- Do not assume that every changing astigmatism prescription is “normal”
- Have a thorough refractive surgery screening before considering LASIK or similar procedures
Long-Term Outlook
The long-term outlook varies. Many patients do well for years with glasses, specialty contact lenses, or cross-linking. Others progress more quickly, especially when diagnosed young. Modern management has significantly improved the outlook because cross-linking can help stabilize progression and specialty lenses can provide much better visual rehabilitation than older options.
The most important strategy is early detection. Keratoconus often causes more trouble when it is discovered late, after substantial corneal distortion has already developed.
Continue Reading
🏁 Take-Home Message
Keratoconus is not just a “strong astigmatism.” It is a structural weakening and distortion of the cornea. Early diagnosis matters. Mild cases may be managed with glasses or contact lenses, but progressive disease may need corneal cross-linking to stabilize the cornea. Because keratoconus affects corneal strength, it is one of the most important conditions to identify before elective refractive surgery.
FAQ
1) What is keratoconus in simple terms?
Keratoconus is a condition in which the cornea becomes thinner and bulges forward, making vision blurry and distorted.
2) At what age does keratoconus usually start?
It is often diagnosed in the teenage years or in young adulthood, although some patients are identified later.
3) Can keratoconus be cured with glasses?
No. Glasses can help vision in early stages, but they do not stop the disease. They correct blur only while you are wearing them.
4) What is the purpose of corneal cross-linking?
Corneal cross-linking is used to strengthen the cornea and help slow or stop progression of keratoconus.
5) Can I have LASIK if I have keratoconus?
Usually, keratoconus is a major warning sign against LASIK and similar tissue-removing corneal laser procedures because the cornea may already be biomechanically weak.
6) Will everyone with keratoconus need a corneal transplant?
No. Many patients do well with glasses, specialty contact lenses, or cross-linking. Corneal transplant is usually reserved for more advanced cases with scarring or poor vision not corrected by other options.
📚 References
- National Eye Institute. Corneal Dystrophies: Keratoconus. Updated December 6, 2024.
- MedlinePlus Medical Encyclopedia. Keratoconus. Updated July 9, 2024.
- NICE. Photochemical corneal collagen cross-linkage using riboflavin and ultraviolet A for keratoconus and keratectasia. Guidance IPG466 / HTG319.
- Mohammadi F, et al. Effectiveness and Safety of Cross-Linking in Keratoconus with Thin Corneas: Systematic Review and Meta-Analysis. 2025.
- Rafizadeh SM, et al. Keratoconus and quality of life: an updated comprehensive review. 2025.
🤝 Roque Eye Clinic Patient Education Series
Dr. Manolette Roque | Dr. Barbara Roque
St. Luke's Medical Center Global City | Asian Hospital Medical Center
Philippines
Medical Review: Roque Advisory Council
Last Updated: March 2026
Medical Disclaimer
This article is intended for educational purposes only and does not replace professional medical consultation.