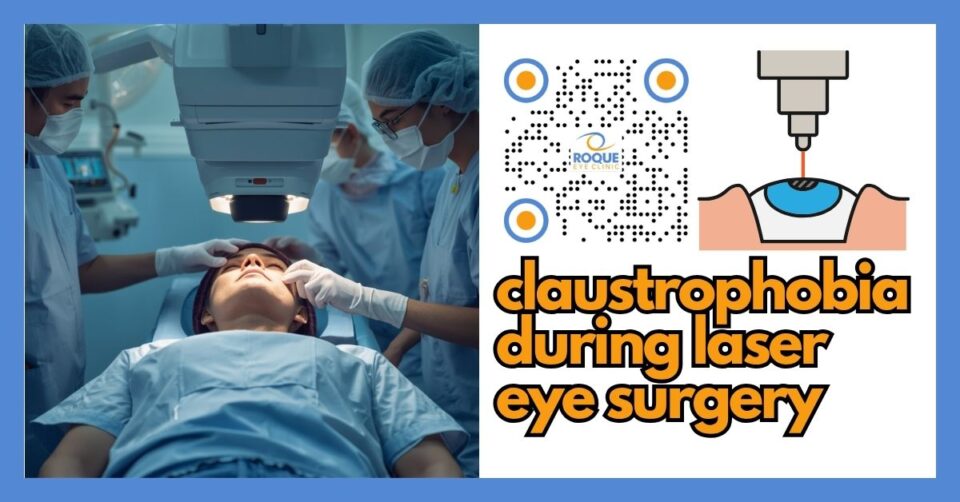
Claustrophobia During Laser Eye Surgery
🧠 Quick Answer
Claustrophobia during laser eye surgery is real, understandable, and important to discuss before treatment. Many patients worry about lying under the machine, keeping still, lights near the eye, or feeling trapped. In most cases, careful counseling, a calm surgical team, step-by-step coaching, and sometimes relaxation medicine can help patients get through the procedure safely and more comfortably.
Laser eye surgery is often quick, but that does not mean it feels emotionally easy for every patient. Some people feel calm and confident. Others become uneasy the moment they imagine lying flat under a machine while someone works on their eyes. For a patient with claustrophobia, panic tendencies, fear of losing control, or strong anxiety around the eye area, the experience can feel much bigger than the surgery itself.
This matters because refractive surgery is elective. The goal is not simply to see whether a procedure can be done. The goal is to decide whether it can be done safely, comfortably, and appropriately for this particular patient. If a patient is likely to panic during the procedure, that deserves serious attention before surgery day.
🧩 Focus: Claustrophobia, anxiety, and panic during laser eye surgery
👁 Goal: Help patients understand why claustrophobia can happen, what the procedure feels like, how surgeons reduce anxiety, and when a different plan may be safer
🛡 Evidence-Based: Preferred Practice Patterns • Standards of Care • Systematic Reviews • Meta-Analyses
ROQUE REFRACTIVE SURGERY Knowledge Hub
Start with the complete guide:
🔬 Claustrophobia During Laser Eye Surgery Anatomy Micro-Primer
- Eyelids: During laser eye surgery, an instrument is used to keep the eyelids open so you do not blink during treatment.
- Cornea: This is the clear front window of the eye. Laser refractive procedures reshape the cornea to change how light focuses.
- Pupil and fixation system: You are usually asked to look at a target light so the treatment stays centered properly.
- Ocular surface nerves: Even though numbing drops are used, the eye still senses pressure, light, dryness, and surface irritation in different ways.
📘 Claustrophobia During Laser Eye Surgery Terminology Glossary
- Claustrophobia: Intense fear of feeling trapped, enclosed, or unable to escape.
- Panic response: A sudden wave of fear that can cause rapid breathing, racing heart, sweating, or an urge to pull away.
- Lid speculum: A small instrument used to keep the eyelids open during surgery.
- Fixation light: The target light the patient is asked to look at during treatment.
- Sedation: Medicine used to help a patient feel calmer or more relaxed.
- Elective surgery: A planned procedure that is chosen, not an emergency operation.
Quick Navigation
Related Reading
Dr. Roque's Key Learning Points
- Claustrophobia during laser eye surgery is not “just nervousness.” For some patients, it can trigger a real panic response.
- Common triggers include lying flat, the machine being close to the face, seeing lights, feeling pressure, and fear of being unable to move or blink.
- Good preoperative counseling can make a major difference because patients usually cope better when they know exactly what to expect.
- Some patients benefit from relaxation medicine, music, breathing coaching, or a slower step-by-step approach.
- If anxiety is severe enough that cooperation is doubtful, postponing or changing the surgical plan may be safer than pushing through.
What Claustrophobia During Laser Eye Surgery Means
Claustrophobia during laser eye surgery usually does not mean the patient is literally afraid of a small room. More often, it means the patient feels trapped by the situation: lying back, staring at a light, having the eyelids held open, sensing the machine close to the face, and knowing that the eye is the focus of the procedure. For some people, that combination creates intense fear even if they understand logically that the procedure is short and controlled.
This is especially important in LASIK and other laser eye procedures because the patient is awake. Official patient information from the FDA and the National Eye Institute explains that patients usually receive numbing drops, may receive medicine to relax, lie on a reclining chair under the laser, are asked to keep fixation on a target light, and may feel pressure or temporary dimming of vision during parts of the procedure. That combination can be unsettling for someone with claustrophobia or panic vulnerability.
💡 Analogy
Imagine being in an elevator that is technically safe, well-lit, and only going up one floor. A person without claustrophobia may find it routine. A person with claustrophobia may still feel trapped the moment the doors close. Laser eye surgery can create a similar emotional reaction: the problem is not only the procedure itself, but the feeling of losing space and control.
Why Claustrophobia Can Happen During Laser Eye Surgery
Several triggers can stack together at once. First, the patient is placed on a reclining chair under a large machine. Second, the surgery is done on the eyes, which many people consider their most vulnerable sense organ. Third, a lid speculum is used to keep the eye open. Fourth, the patient is asked to keep looking at a fixation light rather than pulling away. Fifth, some steps create pressure, dimming of vision, unusual sounds, or odd smells. Any one of these may be tolerable alone, but together they can overwhelm some patients.
Fear during eye surgery is not unusual. A systematic review of cataract surgery performed under local anesthesia found that anxiety is commonly driven by fear of the surgery itself, fear of pain, fear of losing vision, and the sensory experience during surgery. Although cataract surgery and laser refractive surgery are not identical procedures, the emotional pattern is relevant: patients often become more anxious when they do not know what to expect or when they feel they cannot control the situation.
What Patients May Feel During Surgery
Patients describe this in different ways. Some say, “I felt trapped.” Others say, “I knew I was safe, but my body wanted to escape.” Claustrophobic symptoms during laser eye surgery may include rapid breathing, racing heart, sweaty hands, shaking, a feeling of chest tightness, tunnel thinking, or a sudden urge to sit up and stop the procedure. Some patients worry they will move their eye and ruin the surgery. That fear can make the panic worse.
Official FDA patient information also notes that some people feel pressure when suction is applied, may experience temporary dimming of vision, hear ticking sounds from the laser, and notice a smell similar to burning hair as tissue is treated. These sensations do not automatically mean something is wrong, but a patient who is unprepared for them may interpret them as danger signals.
Is Claustrophobia a Contraindication?
Not always. Mild claustrophobia or mild procedure anxiety can often be managed well with good counseling and a thoughtful surgical plan. The question is not whether the patient has ever felt anxious in tight spaces. The real question is whether the patient can remain cooperative and steady enough during the critical parts of surgery.
For example, a patient who says, “I get nervous, but I do well if people explain things to me,” is very different from a patient who says, “I panic during MRIs, I rip masks off my face, and I cannot tolerate having things near my eyes.” The second patient deserves much more careful discussion before proceeding.
Who May Be at Higher Risk
- Patients with known claustrophobia
- Patients with panic disorder or strong panic-like symptoms
- Patients who struggle with MRI scans, dental work, or face masks because of trapped feelings
- Patients who cannot tolerate eye drops, contact lenses, or touching around the eyes
- Patients with trauma history related to the face, restraint, or medical procedures
- Patients who become more anxious when they hear details late instead of early
Why Screening Matters Before Surgery Day
This topic should not first appear while the patient is already on the laser bed. It belongs in preoperative screening and informed consent. A good screening conversation can uncover whether the patient is worried mainly about pain, vision loss, eye instruments, the machine coming close, inability to blink, or loss of control. Once the real trigger is identified, the surgeon and team can decide whether extra reassurance is enough or whether the treatment plan needs modification.
In practical terms, this can be just as important as measuring corneal thickness or pupil size. A technically suitable patient may still be a poor procedural candidate if severe claustrophobia makes cooperation doubtful.
🚨 Emergency Warning
Tell your surgeon before surgery day if you have had panic attacks, severe claustrophobia, trouble tolerating face-level procedures, or a history of pulling away during medical exams. Do not hide this out of embarrassment. Severe anxiety can affect safety and may change the best treatment plan.
How Anxiety Can Be Reduced
1) Step-by-step education
Many patients do better when they know exactly what will happen before it happens. The FDA advises that patients should have the chance to ask questions, review expectations, and not feel pressured into surgery. Education lowers uncertainty, and uncertainty is often what drives panic.
2) Clear intraoperative coaching
Older FDA laser professional-use manuals specifically instruct surgeons to keep the patient relaxed by explaining the process as they go. That point is highly practical. Calm, clear communication during surgery helps the patient feel guided rather than trapped.
3) Relaxation medicine when appropriate
Official patient information from both the FDA and NEI states that some patients may receive medicine to help them relax. This does not replace counseling, but it may help selected patients whose anxiety is moderate rather than overwhelming.
4) Breathing and rehearsal strategies
Simple techniques can help, such as slow exhalation, a pre-agreed stop signal before the critical stage begins, a guided “look at the light and keep breathing” script, or a short dry run in the treatment room before surgery day.
5) Music and supportive environment
The systematic review on surgery-related anxiety found that music and preoperative counseling can improve patient experience. While not every refractive center uses the same protocol, a low-stimulation environment may help the right patient feel less overwhelmed.
What Surgeons Need to Know From the Patient
Patients should be honest. A surgeon needs to know if you have ever stopped an MRI, panicked in a dental chair, fainted during eye drops, or become highly distressed when someone works near your face. These details are not signs of weakness. They are safety information.
It is also helpful to say what makes things easier. Some patients want constant narration. Others want brief cues only. Some need music. Some do better if they practice lying under the machine first. Some need a slower, more deliberate pace. Individualization matters.
When Surgery May Need to Be Postponed
Sometimes the safest decision is to delay. This may happen when the patient cannot tolerate the idea of the laser bed, becomes panicked during practice positioning, cannot fixate steadily enough, or remains too distressed despite counseling. In elective refractive surgery, postponing is not failure. It is a safety decision.
Some patients later proceed successfully after better preparation. Others choose a different refractive option. Some decide they are more comfortable staying with glasses or contact lenses. That is also a valid outcome. The right procedure is the one that matches both the eye and the patient’s ability to undergo it safely.
Questions Patients Should Ask
- What does the machine look like and how close will it be to my face?
- Will I be awake during the procedure?
- Can I be given medicine to help me relax?
- What sensations should I expect, including pressure, dimming, sounds, or smells?
- What happens if I become panicky in the middle of surgery?
- How do you usually help anxious or claustrophobic patients?
Continue Reading
🏁 Dr. Roque's Take-Home Message
Claustrophobia during laser eye surgery is common enough to deserve open discussion before the procedure. Many patients can still do very well with preparation, honest counseling, and the right support. But if panic is likely to overwhelm cooperation, delaying or changing the plan may be safer than forcing an elective surgery that does not feel tolerable to the patient.
FAQ
1) Can you be claustrophobic during LASIK or other laser eye surgery?
Yes. Some patients feel trapped because they are lying under a machine, looking at a light, and having the eyelids held open. Even a short procedure can trigger a panic response in a claustrophobic patient.
2) Will I be asleep during laser eye surgery?
Usually no. Laser refractive surgery is typically done while the patient is awake, with numbing drops. Some patients may also receive medicine to help them relax.
3) What part of the surgery usually triggers claustrophobia most?
Common triggers include the machine being close to the face, the feeling of not being able to blink normally, pressure on the eye, temporary dimming of vision, and fear of not being able to move away.
4) Should I tell my surgeon if I have panic attacks or trouble with MRIs?
Yes. That information is important. It can affect planning, counseling, whether relaxation medicine is considered, or even whether surgery should be postponed.
5) Can medicine help if I am very anxious?
Sometimes yes. Official LASIK information from the FDA and NEI notes that some patients may be given medicine to help them relax. Your surgeon will decide whether that is appropriate for you.
6) If I am too claustrophobic for laser eye surgery, does that mean I failed?
No. Refractive surgery is elective. If the setting feels intolerable, choosing a different plan or postponing is a responsible safety decision, not a failure.
📚 References
- U.S. Food and Drug Administration. What should I expect before, during, and after surgery? LASIK patient information.
- National Eye Institute. Surgery for Refractive Errors.
- Obuchowska I, Konopińska J. Fear and Anxiety Associated with Cataract Surgery Under Local Anesthesia in Adults: A Systematic Review. Clin Ophthalmol. 2021;15:781-795.
- U.S. Food and Drug Administration. Professional Use Information for LASIK systems, including patient fixation and intraoperative coaching guidance.
- National Eye Institute. LASIK Quality of Life Collaboration Project.
🤝 Roque Eye Clinic Patient Education Series
Dr. Manolette Roque | Dr. Barbara Roque
St. Luke's Medical Center Global City | Asian Hospital Medical Center
Philippines
Medical Review: Roque Advisory Council
Last Updated: March 2026
Medical Disclaimer
This article is intended for educational purposes only and does not replace professional medical consultation.