Vitreous Hemorrhage in Diabetes: What It Means, What You May See, and When Surgery Is Needed
🤖 Quick Answer: Vitreous hemorrhage in diabetes happens when fragile abnormal retinal blood vessels bleed into the clear gel inside the eye. It often causes sudden floaters, cobwebs, haze, or major vision loss. Some cases clear with treatment and time, but persistent bleeding, retinal traction, or detachment may require urgent retina care or vitrectomy surgery.
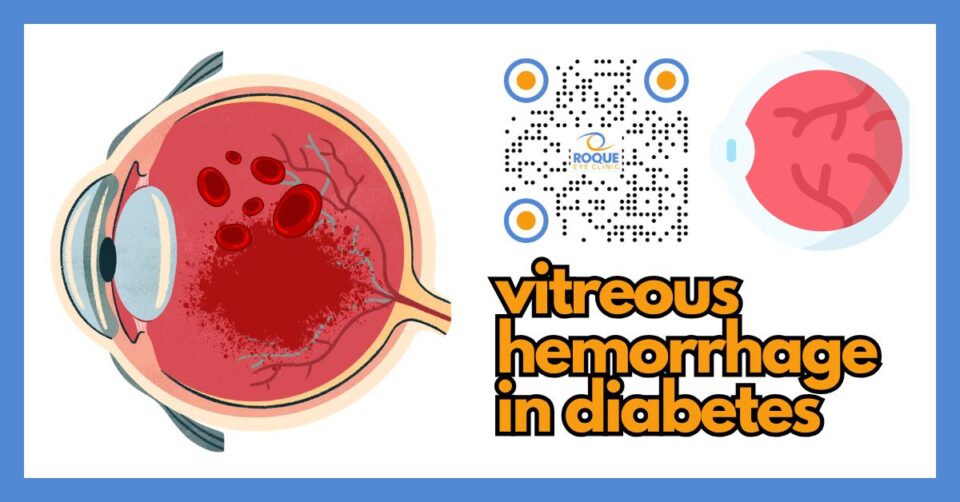
Vitreous hemorrhage means there is bleeding into the vitreous, the clear gel that fills the inside of the eye. In people with diabetes, this usually happens when proliferative diabetic retinopathy creates fragile new blood vessels that easily break and bleed.
For patients, the experience can be frightening. Vision may suddenly look smoky, blurry, full of floaters, or even nearly black. This article explains what vitreous hemorrhage in diabetes is, why it happens, what symptoms to watch for, how retina specialists diagnose it, and when observation, injections, laser, or vitrectomy may be needed.
🧩 Focus: Vitreous hemorrhage caused by diabetic retinopathy
👁 Goal: Help patients understand sudden floaters, haze, and treatment decisions
🛡 Evidence-Based: Preferred Practice Patterns • Standards of Care • Systematic Reviews • Meta-Analyses
🧠 Diabetic Eye Disease Knowledge Hub
Start with the complete guide:
Diabetic Eye Disease: The Complete Patient Guide
🔎 Quick Navigation
- What Is Vitreous Hemorrhage?
- Common Symptoms
- Why It Happens in Diabetes
- Severity and What It May Mean
- How Doctors Detect It
- Treatment Options
- How to Lower the Risk
Related Reading
- Diabetic Eye Disease: The Complete Patient Guide
- Proliferative Diabetic Retinopathy
- Floaters in Diabetic Eye Disease
- Sudden Vision Loss in Diabetes
- Vitrectomy for Diabetic Retinopathy
📌 Key Learning Points
- Vitreous hemorrhage means blood has entered the gel inside the eye.
- In diabetes, it is most often caused by fragile abnormal new vessels from proliferative diabetic retinopathy.
- Typical symptoms include sudden floaters, haze, cobwebs, smoky vision, or major visual drop.
- Some bleeds clear over time, but persistent bleeding, retinal traction, or retinal detachment may require vitrectomy surgery.
- Urgent retina evaluation is important because the eye doctor must rule out tractional or combined retinal detachment.
👁 What Is Vitreous Hemorrhage in Diabetes?
The vitreous is the clear gel that fills most of the inside of the eye. When blood leaks into this gel, it is called a vitreous hemorrhage.
In diabetes, this usually happens in the later stages of diabetic retinopathy, especially when the retina becomes oxygen-starved and starts growing abnormal new blood vessels. These vessels are weak. They can bleed with little provocation, sometimes after coughing, straining, bending, or with no obvious trigger at all.
The amount of blood can vary. A very small hemorrhage may cause only a few floaters. A large hemorrhage may block most or all incoming light and cause dramatic, sudden loss of vision.
👀 Common Symptoms
Symptoms depend on how much blood is present and how close it is to the visual axis. Common patient complaints include:
- Sudden floaters
- Black dots, cobwebs, threads, or pepper-like specks
- Smoky, cloudy, reddish, or hazy vision
- Blurred vision that appears suddenly
- A dark shadow or marked visual drop in one eye
- Difficulty reading, driving, or recognizing faces
Some patients describe it as “looking through dirty water” or “a curtain of black pepper floating inside the eye.” Others may only notice that one eye is suddenly much dimmer than the other.
Sudden floaters, a shower of dark spots, flashes of light, a curtain-like shadow, or rapid vision loss need urgent eye evaluation. In diabetes, these symptoms can mean vitreous hemorrhage, retinal traction, or retinal detachment.
Why Vitreous Hemorrhage Happens in Diabetes
The most common reason is proliferative diabetic retinopathy (PDR). When long-term diabetes damages normal retinal blood vessels, parts of the retina do not get enough oxygen. In response, the eye tries to grow new vessels. Unfortunately, these new vessels are abnormal and fragile.
They may grow on the retina, the optic nerve, or along the back surface of the vitreous. Because they are delicate, they can rupture and bleed into the vitreous cavity.
Vitreous hemorrhage in diabetes may also be associated with:
- Fibrovascular membranes pulling on the retina
- Incomplete prior laser treatment
- Poor blood sugar control
- Long duration of diabetes
- Coexisting hypertension or kidney disease
Related disease background: Diabetic Retinopathy Stages • Non-Proliferative Diabetic Retinopathy • Proliferative Diabetic Retinopathy
Severity and What It May Mean
| Severity | What it usually means | Possible next step |
|---|---|---|
| Mild | A small amount of blood causes a few floaters or mild haze | Retina exam, imaging if possible, close follow-up, treat the underlying retinopathy |
| Moderate | Vision is clearly reduced because blood blocks more of the visual axis | B-scan ultrasound, anti-VEGF in selected cases, laser when view permits, closer monitoring |
| Severe / dense | Heavy bleeding prevents the doctor from seeing the retina well | Urgent retina assessment, ultrasound, possible vitrectomy if non-clearing or if traction/detachment is suspected |
Severity is not judged only by how dark the vision looks. The most important question is whether the eye also has tractional retinal detachment, recurrent bleeding, or high-risk proliferative disease.
🧪 How Doctors Detect It
The diagnosis starts with a detailed history and an eye examination. Your retina specialist will ask when the symptoms started, whether you saw flashes, whether the vision dropped suddenly, and whether you have had previous laser or injections.
Common diagnostic steps include:
- Dilated retinal examination — to assess how much of the retina can still be seen
- B-scan ultrasound — especially important when blood blocks the view of the retina
- Optical Coherence Tomography (OCT) — when possible, to evaluate the macula for associated edema
- Fundus photography — when enough view is available
- Intraocular pressure measurement — to look for pressure-related complications
In dense hemorrhage, B-scan ultrasound becomes especially important because it helps rule out retinal detachment or other hidden posterior segment pathology.
Related diagnostic reads: B-Scan Ultrasound for the Retina • Dilated Eye Exam vs Imaging • OCT for Diabetic Macular Edema
💊 Treatment Options
Treatment depends on several factors:
- How dense the hemorrhage is
- Whether the retina can be seen well enough for laser treatment
- Whether the bleed is clearing on its own
- Whether traction or retinal detachment is present
- Whether the other eye already has severe diabetic disease
1) Observation in selected cases
Some mild or moderate vitreous hemorrhages may clear over time. Blood can slowly settle and the eye can partially reabsorb it. However, “waiting” is only safe when the retina specialist is confident there is no dangerous traction or detachment and when follow-up is reliable.
2) Anti-VEGF injection in selected cases
Anti-VEGF treatment may be used in certain cases of proliferative diabetic retinopathy, including eyes with vitreous hemorrhage. It can help reduce active neovascularization, although it does not replace the need for laser or surgery in every case.
Related reads: Anti-VEGF for Diabetic Eye Disease • Anti-VEGF Injection Procedure • Anti-VEGF Treatment Schedule
3) Laser treatment
If the retina can still be seen well enough, panretinal photocoagulation (PRP) can treat the underlying proliferative disease and lower the risk of further bleeding.
Related read: Laser Treatment for Diabetic Retinopathy
4) Vitrectomy surgery
Vitrectomy may be recommended when the hemorrhage is dense and non-clearing, when bleeding keeps recurring, or when tractional retinal detachment is present or strongly suspected. During surgery, the vitreous gel and blood are removed so the surgeon can clear the visual axis, treat the retina, remove traction, and apply laser internally if needed.
Related reads: Vitrectomy for Diabetic Retinopathy • Vitrectomy Recovery • Tractional Retinal Detachment in Diabetes
5) Systemic control still matters
Even while treating the eye directly, long-term results are better when blood sugar, blood pressure, and other systemic risk factors are managed well.
Related reads: Diabetes Control and Eye Health • Diabetes Targets and Eye Health • Endocrinologist and Diabetic Eye Disease
How to Lower the Risk
Not every vitreous hemorrhage can be prevented, but the risk can be lowered by treating diabetic retinopathy before it reaches the proliferative stage.
- Keep regular diabetic eye examinations
- Do not wait for symptoms before seeking retina care
- Control blood sugar, blood pressure, and lipids
- Complete recommended laser or injection treatment plans
- Return quickly if floaters, haze, or sudden vision loss appears
Prevention and screening reads: Diabetic Eye Exam Schedule • Prevent Diabetic Blindness • Diabetic Retinopathy Screening Programs
Continue Reading
- Proliferative Diabetic Retinopathy
- Tractional Retinal Detachment in Diabetes
- B-Scan Ultrasound for the Retina
- Laser Treatment for Diabetic Retinopathy
- Vitrectomy Recovery
🏁 Take-Home Message
Vitreous hemorrhage in diabetes usually means fragile abnormal retinal vessels have bled into the gel inside the eye. It can cause sudden floaters, haze, or major vision loss.
This is not something to “watch at home” without guidance. Prompt retina evaluation is important because some eyes can be monitored, but others need urgent laser, injections, or vitrectomy surgery.
❓ Frequently Asked Questions
Can a vitreous hemorrhage clear on its own?
Yes. Some mild or moderate hemorrhages may partially clear over time. However, the eye still needs urgent retina evaluation to determine whether there is underlying traction, active proliferative disease, or retinal detachment.
Does a vitreous hemorrhage always mean I need surgery?
No. Some patients can be observed or treated with laser or injections first. Surgery becomes more likely when the bleed is dense, keeps recurring, does not clear, or hides a tractional retinal detachment.
What does diabetic vitreous hemorrhage look like to patients?
Many patients describe black dots, cobwebs, smoky haze, “pepper” in the vision, or a sudden darkening of one eye.
Is vitreous hemorrhage painful?
Usually not. The main symptom is a change in vision rather than pain. If pain is present, the doctor may need to rule out other problems.
Can anti-VEGF injections treat vitreous hemorrhage?
In selected cases, anti-VEGF may help control the abnormal vessels causing the bleed. Still, some eyes will ultimately need laser or vitrectomy depending on severity and underlying traction.
Why is ultrasound important when the eye is full of blood?
Because dense blood can block the doctor’s direct view of the retina. Ultrasound helps detect retinal detachment, traction, and other hidden problems.
📚 References
- American Academy of Ophthalmology. Diabetic Retinopathy Preferred Practice Pattern®.
- American Diabetes Association. Retinopathy, Neuropathy, and Foot Care: Standards of Care in Diabetes—2025.
- National Eye Institute. Diabetic Retinopathy.
- American Academy of Ophthalmology. Summary Benchmarks for Preferred Practice Patterns — Retina/Vitreous.
- StatPearls. Vitreous Hemorrhage.
- StatPearls. Diabetic Retinopathy.
🤝 Roque Eye Clinic Patient Education Series
Reviewed by the Roque Advisory Council
Dr Manolette Roque | Dr Barbara Roque
St Luke’s Medical Center Global City | Asian Hospital Medical Center
Philippines
Medical Review: Roque Advisory Council
Last Updated: March 2026
This article is intended for educational purposes only and does not replace professional medical consultation.
ANIMATION
BOOK AN APPOINTMENT
It takes less than 5 minutes to complete your online booking. Alternatively, you may call our BGC Clinic, or our Alabang Clinic for assistance.