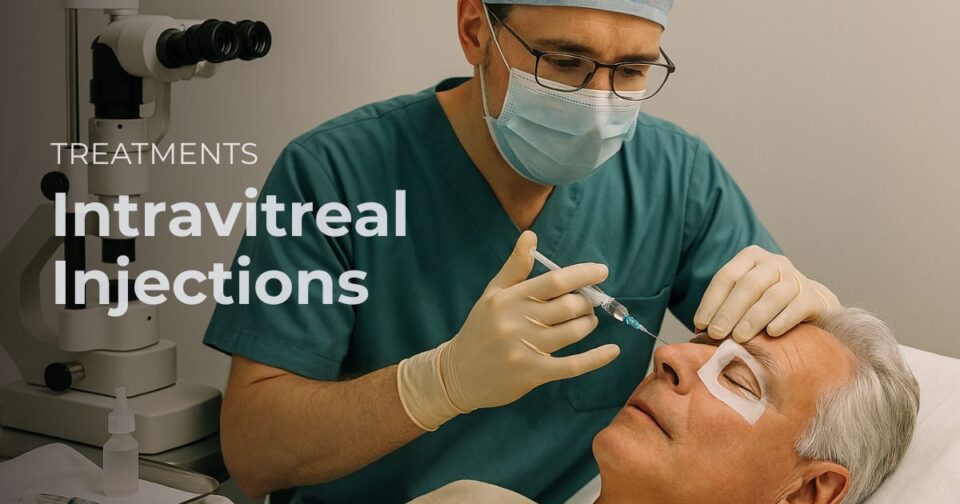
Intravitreal Injections
🧠 Dr. Roque’s Quick Answer
Intravitreal injections are medicines placed directly inside the eye to treat problems at the back of the eye, especially the retina and macula. We commonly use them for wet macular degeneration, diabetic macular edema, diabetic retinopathy, retinal vein occlusion, and some inflammatory or infectious eye problems. The procedure is quick, usually done in the clinic, and is often much less painful than patients expect. The bigger issue is not the injection itself. The bigger issue is whether treatment is started on time and continued consistently.
🎯 Focus
Help patients understand what intravitreal injections are, why they are used, what to expect, and when to seek urgent help after treatment.
👁️ Goal
Reduce fear, improve treatment adherence, and make the next step clear for patients who may need retinal treatment.
🛡️ Evidence-Based
This page follows mainstream retina guidance: intravitreal therapy is a standard treatment pathway for several common retinal conditions and requires follow-up.
Many patients become anxious the moment they hear the words eye injection. That reaction is understandable. However, intravitreal injections are now one of the most important treatments in modern retina care. In the right patient, they can help preserve vision, reduce swelling, slow damage, and sometimes improve sight.
Think of it this way. If the retina is like the camera sensor of the eye, then an intravitreal injection is a way of delivering medicine directly onto the problem area instead of hoping that a drop, tablet, or general treatment will somehow reach the right place in a strong enough dose.
🔎 Quick Navigation
🧩 Anatomy Micro-Primer
The retina is the light-sensitive tissue at the back of the eye. The macula is the part of the retina responsible for sharp central vision, which you use for reading, driving, and recognizing faces. The vitreous is the clear jelly-like space inside the eye. An intravitreal injection places medicine into that vitreous space so the drug can act near the retina and macula.
📘 Terminology Glossary
- Anti-VEGF – Medicines that block signals that cause leaking or abnormal blood vessel growth.
- Macular edema – Swelling in the macula, often from diabetes or blocked retinal veins.
- Wet AMD – A form of macular degeneration involving abnormal leaking blood vessels.
- Retinal vein occlusion – A blockage of a retinal vein that can cause bleeding and swelling.
- Endophthalmitis – A serious infection inside the eye.
- Subconjunctival hemorrhage – A red patch on the white of the eye from a small surface bleed.
What is an intravitreal injection?
An intravitreal injection is a procedure in which medicine is placed directly inside the eye, usually through the white part of the eye using a very fine needle. It is typically performed in the clinic or office setting under sterile preparation and local anesthetic drops.
This is not the same as an injection around the eye, under the skin, or into a blood vessel in the arm. It is a targeted treatment designed for diseases affecting the back of the eye.
Why might you need intravitreal injections?
We usually recommend intravitreal injections when disease at the back of the eye is causing leakage, swelling, abnormal blood vessels, inflammation, or infection that threatens vision. The most common examples include:
- Wet age-related macular degeneration
- Diabetic macular edema
- Diabetic retinopathy with retinal swelling or bleeding risk
- Macular edema from retinal vein occlusion
- Selected cases of uveitis or inflammatory retinal swelling
- Some eye infections that require medicine delivered inside the eye
The core principle is simple: when the disease is inside the eye and near the retina, direct drug delivery is often the most effective way to reach it.
💡 Dr. Roque’s Analogy
If a room in your house has a fire, spraying water on the roof from outside is not a very efficient solution. You want the treatment delivered exactly where the problem is. Intravitreal injections work the same way. They bring the medicine directly to the diseased retinal area instead of relying on a longer and weaker route.
What medicines are given this way?
The most familiar medicines are anti-VEGF drugs. These are often used for wet AMD, diabetic eye disease, and vein occlusion-related swelling. Depending on the case, retinal specialists may also use steroids to reduce inflammation and swelling, or antibiotic, antiviral, or antifungal medicines for severe eye infections.
In real life, the conversation is not just “Do you need an injection?” The real question is “Which medicine is the best fit for your diagnosis, retinal findings, OCT scan pattern, treatment history, response pattern, pressure profile, cataract status, and follow-up reliability?”
Who is a good candidate?
You may be a good candidate if your retinal examination, OCT scan, angiography findings, or clinical history show a condition that is known to respond to intravitreal treatment. A good candidate is not simply someone with blurred vision. A good candidate is someone with a specific retinal diagnosis where timely treatment can realistically protect or improve vision.
This is why a proper retinal assessment matters. Not all blurred vision is retinal swelling. Not all retinal swelling needs the same drug. Not all patients need the same schedule.
What happens during the procedure?
Most intravitreal injections are done in a clinic procedure room or office setting. Your eye will be numbed with drops, cleaned carefully, and kept open with gentle technique so the injection can be given safely. The injection itself usually takes only a few seconds. The full visit is longer because preparation, checking, explanation, and follow-up instructions all matter.
- Your diagnosis and treatment plan are reviewed.
- Numbing drops are placed in the eye.
- The eye and eyelids are cleaned to lower infection risk.
- You are asked to look in a certain direction.
- The medicine is injected through the white part of the eye with a very fine needle.
- Your eye may be checked afterward, depending on the case.
Most patients describe the experience as pressure rather than severe pain. Fear before the first injection is common. After the first one, many patients tell us the anticipation was worse than the actual procedure.
What should you expect after the injection?
Mild irritation, a gritty feeling, tearing, and a small red patch on the white of the eye can happen after treatment. Some patients see tiny bubbles, spots, or floaters for a short time. These are commonly temporary. Vision does not usually improve instantly. The goal is often to reduce retinal swelling or stop further damage over time, not to create an immediate dramatic change within minutes.
In many cases, you can go home the same day and return to routine activity soon after, unless your doctor gives specific restrictions.
What are the risks?
Intravitreal injections are widely used and generally safe, but they are still medical procedures done on the eye. That means risk is real, even if serious complications are uncommon.
Important risks include:
- Infection inside the eye
- Inflammation inside the eye
- Bleeding
- Retinal tear or retinal detachment
- Pressure rise inside the eye
- Corneal surface irritation or abrasion
- Cataract from accidental lens injury in rare cases
That said, the bigger clinical mistake is often undertreatment, delayed treatment, or poor follow-up in a patient whose retina is actively being damaged.
🚨 Dr. Roque’s Emergency Warning
Call your eye doctor or seek urgent ophthalmic care right away if, after an intravitreal injection, you develop:
- Worsening eye pain
- Increasing redness, especially if it keeps getting worse
- Light sensitivity
- Vision that becomes worse instead of better
- Marked swelling or a sudden major change in floaters
These can be warning signs of infection or another serious complication. Do not talk yourself into waiting if the eye is clearly getting worse.
Why are repeat injections often needed?
This is where many patients misunderstand the treatment. Intravitreal injections are often not a one-time cure. They are frequently part of an ongoing treatment strategy.
For example, anti-VEGF treatment commonly begins with a loading phase or close follow-up period. After that, the interval may be adjusted based on your retinal scans, vision, and disease activity. Some patients need monthly treatment at first. Others can later move to longer intervals. Some eventually stop. Others need long-term maintenance to protect vision.
A useful mental model is this: for many retinal diseases, injections are more like blood pressure control than like removing a splinter. They often manage a disease process. They do not always “finish the problem forever” after one visit.
What happens if treatment is delayed?
Delay can matter a lot. In retinal disease, untreated leakage, swelling, bleeding, or abnormal blood vessel activity may permanently damage the macula. That is why we place so much emphasis on timing, follow-up, OCT monitoring, and consistency.
Some patients skip injections because the eye feels “not too bad” that week. That is risky thinking. Retina disease can remain active even when you do not feel much. We treat the disease, not just the day’s comfort level.
How do we decide whether the injections are working?
We do not judge success by guesswork. We look at:
- Your symptoms
- Your visual acuity
- The appearance of the retina on examination
- OCT findings, especially retinal thickness and fluid
- Whether bleeding, swelling, or abnormal vessels are improving
- How long the benefit lasts between injections
A response can be excellent, partial, delayed, or inadequate. In some cases, the plan needs adjustment. That may mean changing the interval, changing the drug, adding laser in selected cases, or considering a steroid-based approach when appropriate.
Common fears patients tell me
“Will I go blind from the injection?”
Serious complications are uncommon, but no intraocular procedure is risk-free. The more honest way to think about it is this: the injection carries a small procedural risk, while the untreated retinal disease may carry a much larger risk to vision.
“Is it very painful?”
Usually, no. Most patients feel pressure, brief discomfort, or irritation rather than severe pain.
“Can I just use drops instead?”
Usually not for these retinal diseases. Eye drops generally do not deliver enough medicine to the back of the eye for this purpose.
“Do I really need more than one?”
Very often, yes. Many retinal diseases are chronic and require repeated treatment or ongoing monitoring.
🧠 Dr. Roque’s Key Learning Points
- Intravitreal injections deliver medicine directly to the back of the eye.
- They are commonly used for wet AMD, diabetic eye disease, and retinal vein occlusion.
- The procedure is quick and usually less painful than patients expect.
- Mild irritation, redness, or a temporary red patch can happen afterward.
- Worsening pain, worsening redness, light sensitivity, or worse vision after injection are danger signs.
- Many patients need repeat injections rather than one treatment only.
- Good follow-up is part of the treatment, not an optional extra.
- Delaying indicated retinal treatment may lead to preventable vision loss.
📚 Related Reading
Frequently Asked Questions
1. Are intravitreal injections done in the operating room?
Usually, no. Most are done in a clinic or office procedure setting using sterile preparation.
2. How long does the injection take?
The actual injection takes only seconds. The full visit is longer because of preparation, explanation, and checks.
3. Will I need someone to accompany me?
That depends on your vision, comfort level, and whether both eyes are being assessed or treated. Many patients still prefer company, especially for the first visit.
4. Can both eyes be treated?
Sometimes, yes. That depends on the diagnosis, the treatment plan, and your retina specialist’s judgment.
5. Are intravitreal injections only for elderly patients?
No. Although wet AMD is more common in older adults, diabetic eye disease, vein occlusion, inflammation, and infection can affect younger patients as well.
6. Can I drive myself home afterward?
Some patients can, but many prefer not to, especially after the first treatment or if vision is already reduced. Follow the advice of your doctor and use common sense.
7. If my eye looks red after the injection, is that always dangerous?
No. A small surface bleed can happen and often looks dramatic but is usually harmless. The important question is whether redness is worsening and accompanied by pain, light sensitivity, or worse vision.
8. What if I miss an injection appointment?
Contact your retina clinic as soon as possible. Do not simply wait for the next month if the treatment was time-sensitive.
9. Can these injections cure my disease permanently?
Sometimes they control the disease very well, but many retinal conditions are chronic. Long-term monitoring is often necessary even when the response is good.
10. Is a scan still necessary if I feel okay?
Yes. Symptoms alone are not enough. OCT and retinal examination often detect activity before patients notice major changes.
✅ Dr. Roque’s Take-Home Message
Intravitreal injections are not something patients should fear more than the disease they are meant to treat. In many retinal conditions, timely injections can be the difference between preserved vision and permanent central vision loss. The injection itself is usually quick. The real success comes from correct diagnosis, proper drug selection, and consistent follow-up. If your retina specialist recommends this treatment, the smart question is not “Can I avoid the injection?” The smart question is “What is the best way to protect my vision from here?”
📖 References
- National Eye Institute. Injections to Treat Eye Conditions. Updated March 24, 2026.
- American Society of Retina Specialists. Intravitreal Injections. Retina Health Series.
- American Academy of Ophthalmology. Intravitreal Injections – 2025 Clinical Statement.
- University Hospital Southampton NHS Foundation Trust. Intravitreal Anti-VEGF Injection Treatment: Patient Information.
- NICE Clinical Knowledge Summaries and treatment guidance for anti-VEGF therapy in wet AMD.
ROQUE Eye Clinic Patient Education Series
Reviewed by the Roque Advisory Council
Dr. Manolette Roque | Dr. Barbara Roque
St. Luke’s Medical Center Global City | Asian Hospital Medical Center
Philippines
Medical Disclaimer: This page is for patient education and general guidance. It does not replace a personal consultation, retinal examination, OCT scan, angiography, or urgent in-person assessment when symptoms are worsening. If you have worsening eye pain, worsening redness, light sensitivity, or worsening vision after an intravitreal injection, seek urgent ophthalmic care immediately.