Uveitis and Ocular Inflammation: Symptoms, Causes, Treatment, and When It Is an Emergency
🧠 Dr. Roque’s Quick Answer
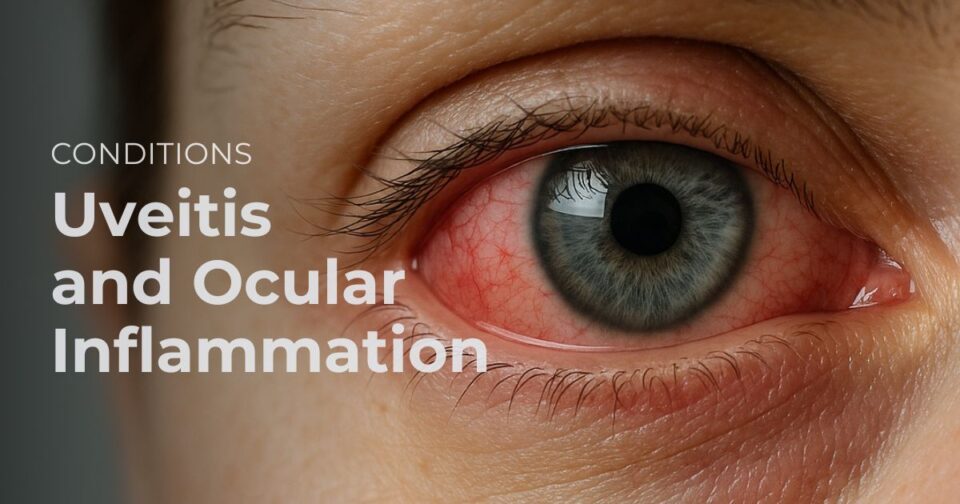
Uveitis means inflammation inside the eye. It is not the same as simple eye strain or ordinary surface irritation. Uveitis can cause redness, pain, light sensitivity, blurred vision, floaters, and even permanent vision loss if it is not treated properly. Some cases are linked to autoimmune disease or infection, while others have no clear cause. Because the stakes are high, suspected uveitis deserves prompt eye evaluation.
Uveitis is one of those diagnoses patients often underestimate because the word sounds unfamiliar. But the real issue is simple: inflammation inside the eye can damage delicate eye structures. That is why a patient with uveitis should not be reassured casually with, “It is probably just red eye.”
The first discipline here is diagnostic humility. A painful, light-sensitive, red eye with blurry vision is not automatically conjunctivitis. If the inflammation is inside the eye, the treatment pathway is very different, and delay can be costly.
🎯 Focus
Explain what uveitis is, why it matters, and how to recognize the patterns that need urgent care.
🏁 Goal
Help patients distinguish routine eye irritation from potentially vision-threatening intraocular inflammation.
🛡️ Evidence-Based
Uveitis can affect the front, middle, or back of the eye and often requires prompt anti-inflammatory treatment plus cause-directed workup.
🧠 Dr. Roque’s Key Learning Points
- Uveitis means inflammation inside the eye, not just irritation on the surface.
- Common symptoms include redness, pain, light sensitivity, blurred vision, and floaters.
- Some cases are linked to autoimmune disease, infection, trauma, medication, or inflammatory conditions elsewhere in the body.
- Not every patient needs the same laboratory workup. Testing should be guided by the clinical pattern, not done randomly.
- Early diagnosis and the right treatment matter because untreated inflammation can lead to cataract, glaucoma, macular edema, scarring, or permanent vision loss.
Quick Navigation
ROQUE Eye Clinic Conditions Knowledge Hub
This article belongs to the Eye.com.ph conditions pathway.
Start with the main hub: Conditions
👁️ Anatomy Micro-Primer
The word uvea refers to the middle vascular layer of the eye. It includes:
- Iris: the colored part of the eye
- Ciliary body: helps the eye focus and contributes to fluid production
- Choroid: the blood-rich layer underneath the retina
In real practice, “uveitis” is used more broadly to describe inflammation that may involve not only the uvea but also nearby structures such as the retina, vitreous, and optic nerve.
🧩 Terminology Glossary
- Uveitis: inflammation inside the eye
- Anterior uveitis: inflammation mainly in the front part of the eye; often called iritis when the iris is involved
- Intermediate uveitis: inflammation centered more in the vitreous or mid-eye region
- Posterior uveitis: inflammation involving the back of the eye, such as the retina or choroid
- Panuveitis: inflammation affecting multiple parts of the eye
- Photophobia: light sensitivity
- Macular edema: swelling of the central retina that can blur vision
- Synechiae: abnormal adhesions involving the iris
What Is Uveitis?
Uveitis is a condition in which the eye develops inflammation inside its tissues. The inflammation may be sudden and dramatic, or it may be quiet, chronic, and harder for patients to notice at first.
Some patients come in with a classic story: a red painful eye, marked light sensitivity, and blurred vision. Others present very differently, especially when the inflammation is deeper in the eye. They may mainly complain of floaters, smudgy vision, or reduced clarity without a striking red eye.
That difference matters. An eye can be seriously inflamed even if it does not look dramatically red from the outside.
Which Part of the Eye Is Inflamed?
One of the biggest clinical mistakes is assuming that all uveitis should look the same. It does not. The location of inflammation changes the symptom pattern, the differential diagnosis, the tests, and the treatment strategy.
💡 Dr. Roque’s Analogy
Think of the eye like a house with several rooms. Inflammation at the front door is easier to notice. Inflammation deep in the back rooms may do more quiet damage before the patient realizes something is wrong. That is why floaters and blurred vision should not be dismissed.
Symptoms of Uveitis
Symptoms vary depending on the location and severity of inflammation, but the most common ones include:
- red eye
- eye pain or aching
- light sensitivity
- blurred vision
- floaters
- reduced vision
- sometimes headache around the eye
Posterior inflammation may produce fewer surface symptoms. So if a patient says, “My eye is not that red, but my vision is cloudy and I am seeing floaters,” you should not relax too early.
What Causes Uveitis?
This is where lazy thinking causes trouble. “Inflammation” is a description, not the final explanation. The real next question is: why is the eye inflamed?
Broadly, uveitis may be linked to:
- Autoimmune or inflammatory disease such as spondyloarthropathy patterns, sarcoidosis, Behçet disease, juvenile idiopathic arthritis, inflammatory bowel disease, and others
- Infection such as herpes virus-related disease, tuberculosis, syphilis, toxoplasmosis, and other infectious causes depending on the clinical pattern and geography
- Trauma or postoperative inflammation
- Medication-related inflammation in selected cases
- Masquerade conditions where something else imitates uveitis
- Idiopathic disease, meaning no specific cause is identified despite proper workup
A hard truth patients should understand: not every case gets a tidy answer. Sometimes we identify the cause clearly. Sometimes we control the inflammation first and continue narrowing the underlying diagnosis over time.
When Uveitis May Be an Emergency
🚨 Dr. Roque’s Emergency Warning
Seek urgent eye evaluation if you have any of the following:
- red eye with significant pain
- red eye with light sensitivity
- sudden blurred vision or reduced vision
- new floaters with hazy or cloudy vision
- known autoimmune disease plus new eye symptoms
- possible eye infection or recent systemic infection
- worsening symptoms despite drops already started elsewhere
Do not self-diagnose uveitis. But also do not under-react to a red painful photophobic eye. The differential diagnosis includes problems that can overlap in presentation, and several of them are vision-threatening.
How We Diagnose Uveitis
A proper diagnosis starts with the pattern. I do not believe in reflexively ordering a random “uveitis panel” for every patient. That approach looks thorough but often produces noise rather than clarity.
The workup usually depends on:
- whether the disease is anterior, intermediate, posterior, or panuveitis
- whether one eye or both eyes are involved
- whether the episode is acute, recurrent, or chronic
- the patient’s age and systemic history
- whether the exam suggests autoimmune, infectious, traumatic, postoperative, or masquerade causes
The eye examination may include slit-lamp evaluation, dilated retinal examination, intraocular pressure measurement, and retinal imaging when needed. Depending on the clinical picture, selected blood tests, imaging, or referral to another specialist may be appropriate.
The disciplined approach
Here is the safer framework:
- Confirm there is real intraocular inflammation.
- Identify where the inflammation is located.
- Decide whether infection must be ruled out quickly.
- Start appropriate control of inflammation.
- Target the workup based on the pattern rather than guessing wildly.
Treatment of Uveitis
Treatment is not one-size-fits-all. The correct treatment depends on the location, severity, recurrence pattern, and suspected cause.
1) Anti-inflammatory treatment
Many cases are treated with anti-inflammatory therapy, often corticosteroids. These may be given as eye drops, injections around or inside the eye, or systemic medication depending on the situation.
2) Cycloplegic or dilating drops
In some cases, drops are used to reduce pain from ciliary spasm and to help prevent complications involving the iris.
3) Infection-directed treatment
If infection is suspected or confirmed, the treatment strategy changes. This is a critical point: steroids alone can be dangerous in the wrong infectious setting. That is why the diagnosis matters so much.
4) Steroid-sparing or immune-modifying treatment
Chronic, recurrent, or severe non-infectious uveitis may require longer-term systemic therapy coordinated with a uveitis specialist and sometimes a rheumatologist or other physician.
5) Monitoring for complications
Control of inflammation is only half the job. We also watch closely for complications such as:
- glaucoma or pressure spikes
- cataract
- macular edema
- posterior synechiae
- retinal damage or scarring
This is why some patients feel frustrated when they hear they need follow-up even after the eye “feels better.” Symptom relief is not always proof that inflammation is fully controlled.
Can Uveitis Cause Permanent Vision Loss?
Yes, it can. That is the uncomfortable but important truth. Vision loss may occur from the inflammation itself or from complications such as macular edema, glaucoma, cataract, retinal injury, or optic nerve involvement.
The good news is that many patients do well when the disease is recognized early, monitored carefully, and treated appropriately. The mistake is delay, not caution.
What Patients Often Get Wrong
- They assume a red eye is always conjunctivitis.
- They assume no discharge means no serious problem, which is false.
- They underestimate floaters and cloudy vision when the eye is not very red.
- They self-medicate with leftover drops.
- They stop follow-up too early when symptoms improve.
The disciplined patient wins by doing the opposite: get examined, follow the treatment plan, return for follow-up, and tell the doctor about systemic illnesses, joint pain, skin disease, bowel disease, infections, travel risk, or immune problems.
When to Book a Consultation
Book an eye consultation promptly if you have a painful red eye, unusual light sensitivity, blurred vision, new floaters, recurrent episodes of eye inflammation, or a known autoimmune condition with new ocular symptoms. If symptoms are significant or worsening, do not wait for them to “settle down on their own.”
✅ Dr. Roque’s Take-Home Message
Uveitis is not just “eye redness.” It is inflammation inside the eye, and it can threaten vision if it is ignored or treated incorrectly. The safest move is prompt diagnosis, careful follow-up, and treatment that matches the actual cause. If you have redness with pain, light sensitivity, blurred vision, or floaters, take it seriously.
Frequently Asked Questions
Is uveitis the same as conjunctivitis?
No. Conjunctivitis affects the surface lining of the eye, while uveitis is inflammation inside the eye. The implications and treatment are different.
Can uveitis happen without much redness?
Yes. Deeper forms of uveitis, especially posterior disease, may present more with floaters or blurred vision than with dramatic redness.
Is uveitis always caused by autoimmune disease?
No. It can be linked to autoimmune disease, infection, trauma, medications, surgery, or no clearly identified cause.
Can stress cause uveitis?
Stress may affect how patients experience symptoms, but true uveitis is not diagnosed by blaming stress alone. Real inflammation inside the eye needs proper examination.
Can uveitis come back?
Yes. Some patients have recurrent disease, which is one reason careful follow-up matters.
Do all patients need blood tests?
No. Testing should be targeted to the pattern and suspected cause. Random broad testing is often low-yield.
Can steroid drops fix everything?
No. Steroids are important in many cases, but they are not a substitute for diagnosis. Infection and other causes may need different treatment.
Can uveitis cause glaucoma?
Yes. The inflammation itself, scarring, or some treatments can raise eye pressure and lead to glaucoma risk.
Can children get uveitis?
Yes. Pediatric uveitis exists and can be especially important because it may be quiet yet vision-threatening.
When should I worry most?
Worry more when symptoms include pain, light sensitivity, reduced vision, floaters, recurrent inflammation, or a known systemic inflammatory disease.
📚 Related Reading
📖 References
- American Academy of Ophthalmology. Patient and professional educational resources on uveitis and anterior uveitis.
- National Eye Institute. Uveitis overview and treatment information.
- EyeWiki. Treatment of Uveitis and Acute Anterior Uveitis.
- MedlinePlus Medical Encyclopedia. Uveitis overview.
- Standard ophthalmology references on intraocular inflammation, pattern-based diagnosis, and complication monitoring.
ROQUE Eye Clinic Patient Education Series
Reviewed by the Roque Advisory Council
Dr. Manolette Roque | Dr. Barbara Roque
St. Luke’s Medical Center Global City | Asian Hospital Medical Center
Philippines
Medical Disclaimer: This page is for patient education only and does not replace a complete eye examination, diagnosis, or treatment plan. If you have eye pain, light sensitivity, a red eye with blurred vision, or new floaters, seek prompt medical evaluation.